
Additionally, a variety of OTC products are available only at the military hospitals and clinics. TRICARE is unique in that a limited number of over-the-counter drugs are included on the formulary and available all three points of service. The DOD beneficiary formulary change communication process is driven by the recommendations found in the published DOD P&T committee meeting minutes 3. Examples include removal of a drug from the formulary (Tier 4 status), an increase in the cost-share (Tier 3 status), and a change from a preferred to a non-preferred status, which can include but is not limited to new step therapy or pre-authorization requirements. Patient-specific notification letters are mailed to beneficiaries impacted by a variety of formulary changes. 
Although the 2000 NDAA directed patient notification to inform beneficiaries of pharmaceutical agents changing formulary status to Tier 3 or (nonformulary status), it became apparent that communication on several other formulary actions (e.g., prior authorization criteria, Tier 4 designation) were also needed.īeginning in October 2007, the DOD has taken key steps to improve communication with beneficiaries concerning formulary changes. Given the variety of formulary changes that have occurred over the years, communication to impacted beneficiaries is essential. Providers and beneficiaries can refer to the TRICARE formulary search tool 2 for information on tiered copay status and other requirements, including prior authorization or quantity limits. The P&T committee not only evaluates drugs for exclusion from coverage, but also identifies branded drugs that may be moved to Tier 1 status with a lower copayment for beneficiaries. 
Similar to commercial pharmacy benefit plans, beneficiaries must pay the full out-of-pocket cost for Tier 4 drugs at retail network pharmacies and these agents are not available at military hospitals or clinics or TRICARE Mail Order pharmacy. Since its creation, the TRICARE Uniform Formulary has evolved considerably. In 2018, the NDAA directed TRICARE to add a fourth “not covered” tier to its formulary, which excludes coverage of pharmaceutical agents that have little clinical effectiveness. 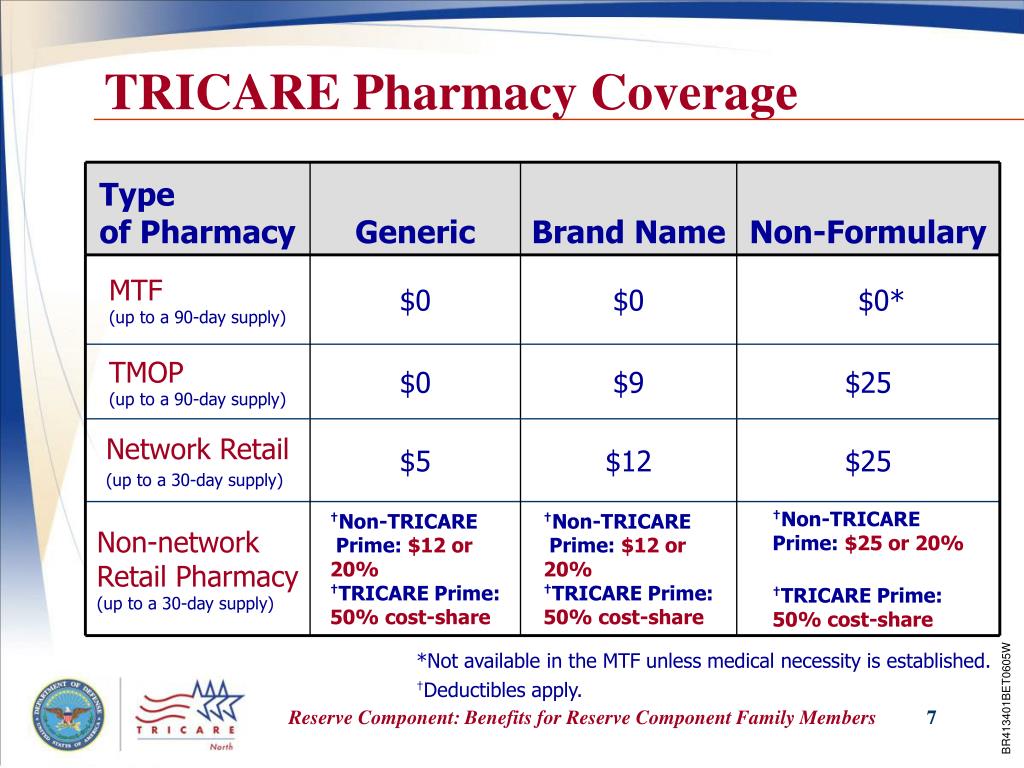
Following the BAP comments, the final formulary decisions are reviewed and signed by the director of the Defense Health Agency. The BAP is unique in that it gives beneficiaries a voice in what medications are included on the formulary, while providing transparency to what is often an unpublicized process in other health systems. Federal law requires that the BAP review and comment on the DOD P&T committee recommendations for implementing formulary changes to Tier 3 status, pre-authorization criteria, and implementation periods. The DOD P&T committee recommendations are then discussed publicly with the Beneficiary Advisory Panel, which is comprised of nongovernmental organizations representing DOD beneficiaries, pharmacy contractors and TRICARE network providers. The pharmacy tiered copays are based on the point of service and formulary status (generic, formulary brand and nonformulary agents), with the Tier 3 (nonformulary) copay being the most expensive. The outpatient TRICARE pharmacy benefit evaluates several components including prior authorization criteria, step therapy, quantity limits, formulary status, and a tiered copay structure. The Department of Defense P&T committee meetings are held quarterly, with recommendations determining which medications are included on the Uniform Formulary based on clinical and cost-effectiveness of the agents. The TRICARE Uniform Formulary provides three points of service for prescription dispensing and includes military hospitals and clinics worldwide, one TRICARE Mail Order Pharmacy (home delivery) and retail network pharmacies located in the United States and several U.S. The National Defense Authorization Act for Fiscal Year 2000 required the establishment of a Pharmacy and Therapeutics committee to develop and maintain a Uniform Formulary of medications-a list of brand name and generic drugs and supplies that TRICARE covers-which provides pharmacy benefits in the outpatient setting. TRICARE is the health care program that provides coverage to 9.6 million uniformed service members, retirees, and their family members.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
